So, you’ve finally decided to join a medical aid. Maybe you’ve landed a full-time gig, started a family, or just realised that private hospital bills are no joke. Whatever your reason, welcome! But if you’re joining a little later in life or after being uncovered for a while, you might bump into two confusing terms: waiting periods and late joiner penalties.

Babies are expensive. We're talking “a pram that costs more than your first car” expensive. “R900 organic cotton onesie with ‘Cute or what?’ embroidered on it” expensive. But most of all? Private hospital expensive. Specialist expensive. “Sorry, your medical aid doesn’t cover the full amount” expensive.

While you may have some form of medical aid plan, depending on its structure, more often than not the scheme will not cover all the doctor and other specialist fees, or all procedures in hospital. Medical gap cover pays the difference between the medical aid rates and the higher actual cost charged.


Navigating adulthood means managing expenses for essentials like Medical Aid—a necessity that often feels like a burden until it’s needed. Hippo simplifies the process, saving you time and money by comparing top plans in minutes. Discover how to protect your health and wallet with ease. Adulting doesn’t have to be hard—Hippo is here to help!






Laughter may be the best medicine, but when it comes to staying healthy, there’s no substitute for proper medical aid. Whether it’s a late-night trip to the ER or a routine check-up, knowing you have the right coverage offers peace of mind when you need it most. At Hippo, we’re here to simplify the process of finding a medical aid plan that fits your needs and budget, ensuring you can focus on what matters most—your health, without worrying about unexpected costs.





It might be the perfect time to review your Medical Aid policy and decide whether you’ll need to upgrade or downgrade your current plan. But, deciding on the right scheme or plan can be daunting, as you’re constantly bombarded with Medical Aid jargon. Luckily, this year you’ll be in the know. We’ve taken a closer look at some Medical Aid terms to help you understand what they mean, so you can make an informed decision.

The South African Council for Medical Schemes has just announced their suggested increase percentage margin (5% + utilisation) for the 2023/2024 medical aid scheme premium increases coming up. Let's find out what that means for you and if there's anything you can do to ease the impact of coming changes on your pocket.



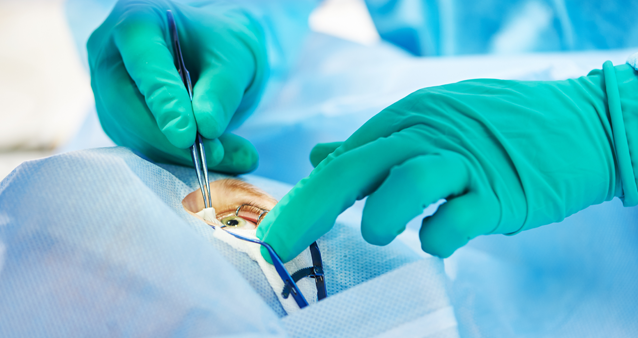
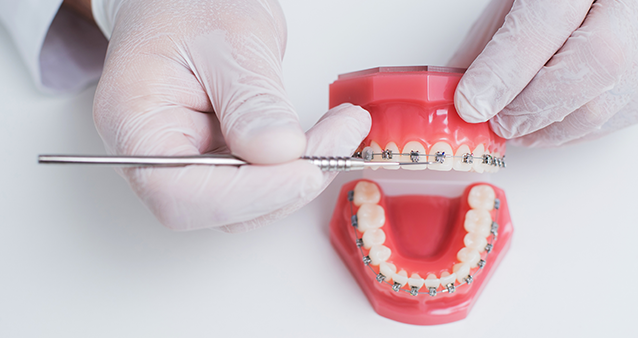

In the grand scheme of life, you don't have to worry about trying to decipher the difference between a medical aid and a hospital plan. We know it can feel like you are trying to understand why the chicken crossed the road - we all think we know, but do we really? That's where hippo.co.za comes in to save the day. Let's start with the basics.


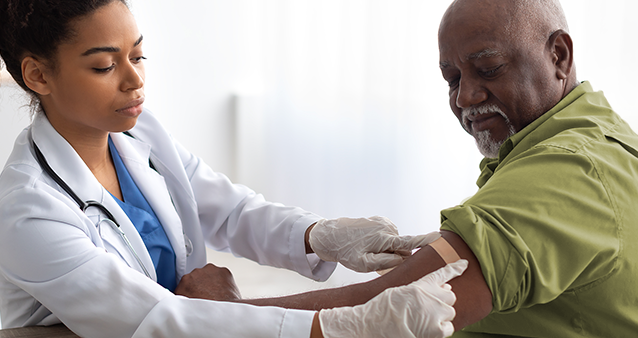








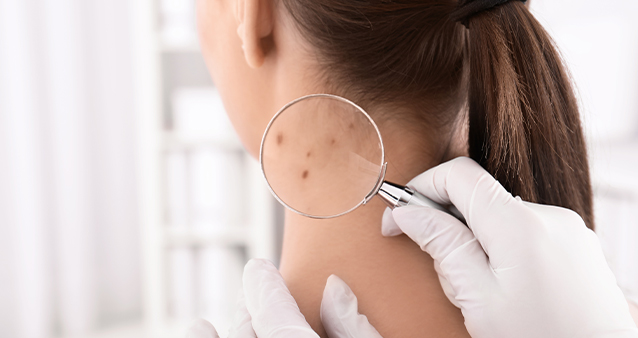





COVID-19 treatment has been listed as a Prescribed Minimum Benefit (PMB) condition for medical scheme members by the Council for Medical Schemes (CMS). But what does this mean for you if you get 'long COVID', where you find yourself still experiencing symptoms months after you 'recover' from the initial period of sickness? Will your medical aid cover you?




The majority of people are on medical aid plans that cover in-hospital specialists' charges at 100% of the medical aid rate. In most instances, specialists charge more than 100% of the medical aid rates, potentially leaving you with a shortfall that you have to pay from your pocket. Depending on your medical aid plan, you may be covered for up to 300% of the scheme rate. This means that if the specialist's charges for in-hospital expenses are three times the general medical aid rate, your medical aid is sufficient. Medical gap cover is an insurance that will fill in the difference, should the specialist's charges be higher, rather than leaving you with what could be a large bill.









In 2020, savvy consumers are looking to cut costs, scale down, and consume less. From clothes to cars, we're always on the hunt for the best value for money, and it should be no different with our medical aid. But making medical aid decisions is less fun and more cumbersome than choosing a SUV and takes a little discipline.


It’s hard to believe that 2009, the year that Avatar was the most popular movie and people danced to the Black Eyed Peas’ Boom Boom Pow, was 10 years ago. In that time, many fad diets have come, gone, and come again. Food science has changed vastly in the past few decades and has caused many heated debates on what’s healthy and unhealthy for the human body. Confusingly, different studies and research support both sides of food debates, so it’s hard to know what and how we should eat.

Being pregnant is a wonderful time which shouldn’t be overshadowed by worrying about how you’re going to afford being a parent. While medical aid may go a long way to help manage the costs of pre- and post-natal care, there are other expenses that you can be prepared for to ensure your pregnancy is nine months of bliss.

Your lives are busy. With work, family, and friends, making quality time can be difficult for many couples. When your baby arrives, having time to connect with your partner alone will be nearly impossible for a while. On a babymoon, it’s just the two of you to help strengthen your relationship even more.
Worldwide, one in every three women and one in every five men over 50 years old will fracture a bone due to osteoporosis, a progressive disease that causes bones to become weak and brittle. It occurs in one of two ways – either bones lose their density or the body doesn’t make enough bone. Either way, this forms large holes and spaces within bones and makes them easily breakable.

With smartphone adoption at an all time high, we have the world at our fingertips. A swipe of the screen and a touch of a button later, we’ve got all the information we need at any given time. While this has certainly made our lives easier in some regards, it has also led to an overload of information as we check our phones and tablets throughout the day, even when we’re out with friends.

There are certain money mistakes that can cost you for the rest of your life, such as taking on too much debt or failing to save enough for your retirement. Ensure you remain financially stable by avoiding the following five money mistakes from a list compiled by three financial advisors who work with people and their money every single day

If you have ever volunteered your time before, you might have noticed a mood lift, or bursts of satisfaction, happiness and elation. Volunteering is an unselfish act of giving of your free time and resources to those who need your help, and in due course you may experience the results of all your efforts, and even build a community of friends with whom you enjoy a shared interest and passion.

Tax return season for individuals officially opened on 1 July 2017. If you are a South African citizen, you may need to submit an income tax return to the South African Revenue Service (SARS) over the next couple of months (deadlines to be announced). The purpose of filing an income tax return is for SARS to determine how much money you owe the government or if you're due for a tax rebate.

While conventional wisdom tells us to stay away from meals served in foam containers or paper wraps, not all unhealthy food is bad for one's health. Hippo.co.za reached out to two nutrition experts to find out which foods, snacks and beverages traditionally considered dietary no-no's, may actually have positive health outcomes when taken in very limited portions and cooked the right way.

It’s an inevitable part of being a parent that at some point you’ll have a sick child on your hands. For more serious illnesses like chickenpox or ear infections, you’ll probably have to make a trip to the doctor, but for minor things like scrapes and cuts, sniffles and tummy bugs you can usually buy over-the-counter medicine to help relieve your little one’s discomfort.

In the past, holidays were all about working on your tan, lounging by the swimming pool and eating too many pastries at the restaurant’s buffet. But, with the growing worldwide trend of personal health and wellness on the rise, holidays have become about much more than that – they’ve become another chance to work on your long-term health, another health investment on top of your Medical Aid plan.
Many of us fear being diagnosed with common diseases such as cancer or diabetes, but for a small percentage of the population, visiting a doctor has yielded more terrifying results. More people than you might think, worldwide, suffer from strange and shocking illnesses, many of which you may never have heard of. In this article, you’ll learn more about these conditions, which continue to perplex the medical industry.

Are you aware of what you're eating? Of course you are, otherwise you wouldn't have ordered your favourite burger from your local fast food outlet. But do you know what it consists of? It may just seem like a tasty compilation of a bun, beef patty, cheese and tomato, but there may be more to that burger than meets the eye.

As we run between cubicles and stare at LED monitors for hours on end, we often forget that South Africa is a land of adventure, filled with unforgettable journeys - but it's up to you to embark on them. The holiday season is fast approaching and with the weather warming up, it is a perfect time to experience some of the greatest treks in South Africa.

We all have different needs when it comes to our health and Medical Aid scheme. While you may have been with your current Medical Aid provider for quite some time now, it might be a good idea to review your current plan and ask the right questions such as how its provisions suit your current state of health.





Hippo Blog Categories